Navigating 2026 Medicaid Updates: 5 Key Changes for Family Caregivers in the United States
For millions of family caregivers across the United States, understanding and adapting to changes in healthcare policy is not just a matter of compliance, but a fundamental aspect of providing the best possible care for their loved ones. As we approach 2026, the landscape of Medicaid is set to evolve, bringing with it a series of significant updates that will directly impact how family caregivers operate, what services are available, and the financial considerations involved. These 2026 Medicaid Updates are not merely bureaucratic adjustments; they represent a shift in the way long-term care, home-based services, and financial assistance are structured and accessed. Being prepared and informed about these changes is paramount to ensuring continuity of care and maximizing the support available.
The role of a family caregiver is often demanding, requiring immense dedication, emotional resilience, and a keen understanding of complex systems. From managing daily medical needs to navigating intricate financial paperwork, caregivers wear many hats. The impending 2026 Medicaid Updates will add another layer of complexity, but also potentially open new avenues for support. This comprehensive guide aims to break down the five most crucial changes that family caregivers need to be aware of, offering actionable insights and practical advice to help you navigate this evolving terrain. We will delve into how these updates might affect eligibility, service delivery, financial planning, and the overall support system for both caregivers and recipients.
Understanding these adjustments now can empower caregivers to proactively plan, advocate effectively for their loved ones, and ensure that they continue to receive the necessary care without interruption. Let’s explore the critical aspects of the 2026 Medicaid Updates and what they mean for you and your family.
1. Expanded Eligibility Criteria and Income Threshold Adjustments
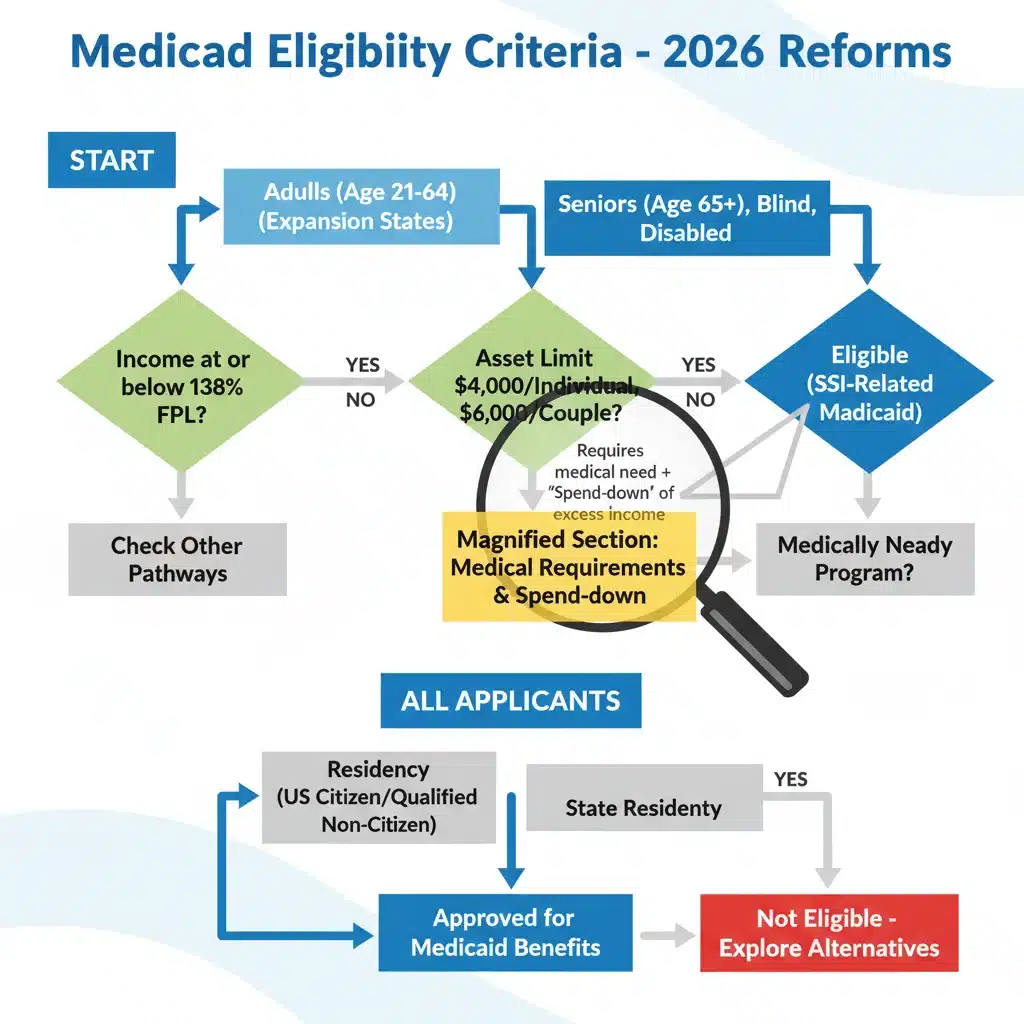
One of the most anticipated aspects of the 2026 Medicaid Updates revolves around potential changes to eligibility criteria and income thresholds. Medicaid, as a joint federal and state program, provides health coverage to millions of Americans, including low-income adults, children, pregnant women, elderly adults, and people with disabilities. The specifics of eligibility can vary significantly from state to state, but federal guidelines often set the baseline for these programs. The 2026 updates are expected to bring about revisions that could either expand access for more individuals or introduce stricter requirements, depending on legislative outcomes and economic forecasts.
What to Expect:
- Income and Asset Limits: There’s a strong possibility that income and asset limits for certain Medicaid programs, particularly those related to long-term care, may be adjusted. These adjustments could be influenced by inflation, federal poverty level changes, and state budget considerations. For family caregivers, this means carefully re-evaluating their loved one’s financial situation against the new benchmarks. Even slight changes can impact eligibility for critical services.
- Medically Needy Pathways: Some states might introduce or expand “medically needy” pathways, allowing individuals with high medical expenses to qualify for Medicaid even if their income is above the standard limit. This could be a lifeline for families facing significant out-of-pocket costs for chronic conditions or disabilities. Caregivers should research their state’s specific provisions in this area.
- Spousal Impoverishment Rules: These rules are designed to prevent the spouse of a Medicaid recipient who needs long-term care from becoming impoverished. The 2026 Medicaid Updates might see modifications to the Community Spouse Resource Allowance (CSRA) or the Minimum Monthly Maintenance Needs Allowance (MMMNA). Understanding these rules is crucial for married couples to protect assets for the non-Medicaid spouse while still qualifying for necessary care.
- Home and Community-Based Services (HCBS) Waivers: Many states utilize HCBS waivers to provide care in a person’s home or community, rather than in an institution. Eligibility for these waivers often has its own set of criteria, which may also be updated. These waivers are incredibly important for family caregivers who wish to keep their loved ones at home, offering services like personal care, skilled nursing, and respite care.
Impact on Family Caregivers:
These changes directly affect whether a loved one qualifies for Medicaid, which in turn dictates the level of financial assistance and services available. Caregivers will need to stay vigilant about state-specific announcements regarding these thresholds. It might require proactive financial planning, asset protection strategies, or even exploring alternative funding sources if eligibility becomes more restrictive. Conversely, expanded eligibility could alleviate significant financial burdens, making it easier to afford necessary care.
To prepare, family caregivers should begin gathering financial documents, reviewing current assets and income, and consulting with elder law attorneys or financial advisors specializing in Medicaid. Understanding the nuances of these changes will be key to ensuring uninterrupted care and financial stability.
2. Enhanced Focus on Home and Community-Based Services (HCBS)
A significant trend in healthcare policy, which is expected to be further solidified by the 2026 Medicaid Updates, is the continued emphasis on Home and Community-Based Services (HCBS). There’s a growing recognition that many individuals prefer to receive care in their homes or communities rather than in institutional settings like nursing homes. HCBS programs not only improve the quality of life for recipients but can also be more cost-effective for states in the long run.
Key Developments:
- Increased Funding and Access: Federal initiatives are likely to infuse more funding into HCBS programs, potentially leading to an expansion of available services and a reduction in waiting lists for waivers. This could mean more people getting access to care coordinators, personal care aides, adult day health services, and home modifications.
- Service Expansion: The range of services covered under HCBS waivers may broaden. This could include greater access to assistive technology, transportation services, behavioral health support, and even caregiver training and support programs. For family caregivers, this means a wider array of resources to help them manage their responsibilities and prevent burnout.
- Caregiver Support Programs: A critical component of enhanced HCBS is often the direct support provided to family caregivers. The 2026 Medicaid Updates could see an increase in programs offering respite care, training on specific medical tasks, counseling, and financial stipends for family members providing care. These programs acknowledge the invaluable role of unpaid caregivers and aim to sustain their ability to provide care.
- Person-Centered Planning: Expect a continued push towards person-centered planning, where the care plan is tailored specifically to the individual’s needs, preferences, and goals. This approach empowers recipients and their families to have a greater say in the services they receive, fostering a more collaborative care environment.
Impact on Family Caregivers:
The strengthening of HCBS is overwhelmingly positive for family caregivers. It provides more options for keeping loved ones at home, reduces the financial strain associated with institutional care, and offers direct support to caregivers themselves. However, navigating the various HCBS waivers and programs can be complex. Each state has its own set of waivers, with different eligibility requirements and covered services. Caregivers will need to become familiar with their state’s offerings and understand how to apply.
Proactive steps include researching state-specific HCBS programs, understanding the application process, and advocating for the specific services needed. Connecting with local Area Agencies on Aging or disability organizations can provide invaluable guidance and support in accessing these vital resources.
3. Greater Emphasis on Value-Based Care and Quality Measures
The healthcare system as a whole is moving towards a value-based care model, where providers are reimbursed based on the quality of care and patient outcomes, rather than simply the volume of services provided. The 2026 Medicaid Updates are expected to integrate more of these principles into Medicaid programs, particularly in long-term care and managed care organizations.
Anticipated Changes:
- Performance-Based Reimbursement: States may implement or expand performance-based payment models for providers of long-term care services. This means that nursing homes, home health agencies, and other providers could receive incentives for achieving specific quality metrics, such as reduced hospital readmissions, improved patient satisfaction, or better management of chronic conditions.
- Enhanced Quality Reporting: Expect more rigorous reporting requirements for healthcare providers to demonstrate the quality of their services. This data will be used to evaluate provider performance and inform policy decisions. For caregivers, this could translate into greater transparency regarding the quality of care available from different providers.
- Managed Care Expansion: Many states utilize Medicaid Managed Care Organizations (MCOs) to deliver services. The 2026 Medicaid Updates might see an expansion of MCOs, with a stronger focus on integrating physical health, behavioral health, and long-term services and supports within these plans. MCOs often have their own care coordination services, which can be beneficial to caregivers.
- Patient Outcome Measures: There will likely be a continued focus on measuring patient outcomes, such as functional independence, community integration, and overall well-being. This shift aims to ensure that Medicaid funds are being used effectively to improve the lives of beneficiaries.
Impact on Family Caregivers:
While the goal of value-based care is to improve quality, the immediate impact on family caregivers can be varied. On the one hand, it could lead to better quality of care from providers who are incentivized to perform well. On the other hand, navigating new quality metrics and understanding how they affect service delivery might require additional effort from caregivers. It also places a greater emphasis on choosing providers who consistently meet high standards.
Caregivers should actively engage with providers, ask questions about their quality measures and outcomes, and provide feedback on the care received. Becoming an informed advocate for quality care is more important than ever. Understanding how MCOs operate in your state, if applicable, and how to utilize their care coordination services will also be beneficial.
4. Digital Transformation and Telehealth Integration
The accelerated adoption of telehealth during the recent public health crisis has demonstrated its immense potential for delivering healthcare services efficiently and conveniently. The 2026 Medicaid Updates are expected to solidify and expand the integration of digital health solutions and telehealth services within the Medicaid framework.
Innovations to Watch For:
- Permanent Telehealth Coverage: Many temporary telehealth flexibilities introduced during the pandemic are likely to become permanent. This means continued coverage for a wide range of services delivered via video or phone, including doctor’s appointments, mental health counseling, and certain therapy sessions.
- Remote Patient Monitoring (RPM): The use of RPM devices, which allow healthcare providers to monitor a patient’s health data from a distance, is expected to grow. This can be particularly beneficial for individuals with chronic conditions, enabling early intervention and reducing the need for emergency room visits. Medicaid coverage for RPM devices and services could expand.
- Digital Health Literacy Programs: Recognizing that not everyone has equal access to or comfort with technology, there may be initiatives to improve digital health literacy among Medicaid beneficiaries and their caregivers. This could include resources and training to help families utilize telehealth effectively.
- Streamlined Digital Access: Efforts to streamline online application processes, digital portals for managing benefits, and electronic health records will likely continue. The goal is to make accessing and managing Medicaid benefits more user-friendly.
Impact on Family Caregivers:
Telehealth and digital transformation offer significant advantages for family caregivers, particularly those living in rural areas or balancing caregiving with work and other responsibilities. It can reduce the need for transportation, save time, and provide more flexible access to healthcare professionals. For instance, a caregiver might be able to participate in a doctor’s appointment remotely, or their loved one could receive therapy sessions from the comfort of their home.
However, it also presents challenges, such as ensuring reliable internet access, having the necessary equipment (like smartphones or computers), and digital literacy. Caregivers will need to embrace these technological advancements and advocate for resources that support their adoption. Understanding how to schedule and participate in telehealth appointments, and how to utilize remote monitoring tools, will become increasingly important.

5. Increased Scrutiny and Anti-Fraud Measures
As Medicaid programs continue to expand and evolve, there is often an accompanying increase in efforts to prevent fraud, waste, and abuse. The 2026 Medicaid Updates are likely to include strengthened measures to ensure the integrity of the program, which can have implications for both providers and beneficiaries, including family caregivers.
Potential Anti-Fraud Initiatives:
- More Robust Verification Processes: Expect more stringent verification processes for eligibility and service utilization. This could involve more frequent reviews of financial information, residency, and medical necessity. While designed to prevent fraud, these measures can sometimes add administrative burdens for legitimate beneficiaries and their caregivers.
- Data Analytics and Technology: States will likely leverage advanced data analytics and artificial intelligence to detect patterns indicative of fraudulent activity. This proactive approach aims to identify and address issues before they become widespread.
- Provider Audits and Oversight: Increased auditing of healthcare providers who bill Medicaid is anticipated. This ensures that services are being rendered appropriately and that billing practices are compliant with regulations.
- Education and Outreach: Alongside enforcement, there may be increased efforts to educate beneficiaries and caregivers about what constitutes fraud and how to report suspicious activities. Empowering individuals to recognize and report potential issues is a key part of prevention.
Impact on Family Caregivers:
While anti-fraud measures are essential for protecting taxpayer dollars and ensuring the sustainability of Medicaid, they can sometimes create additional paperwork and scrutiny for family caregivers. It’s crucial for caregivers to maintain meticulous records of all medical care, financial transactions, and communications related to their loved one’s Medicaid benefits. Any discrepancies or incomplete documentation could lead to delays or challenges in receiving services.
Caregivers should be diligent in understanding their responsibilities regarding documentation and reporting. If you employ a personal care aide or other service provider through Medicaid, ensure they are properly credentialed and that their services are accurately recorded. Staying informed about your state’s specific anti-fraud initiatives and knowing who to contact for clarification or to report concerns is vital. Transparency and accuracy in all dealings with Medicaid will be your best defense against potential issues.
Preparing for the 2026 Medicaid Updates: A Caregiver’s Checklist
The upcoming 2026 Medicaid Updates represent a significant juncture for family caregivers. Proactive preparation is the most effective way to navigate these changes smoothly. Here’s a checklist to help you get started:
- Stay Informed: Regularly check official state Medicaid websites, federal government health portals (like Medicaid.gov), and reputable caregiving organizations for updates. Subscribe to newsletters and participate in webinars.
- Review Eligibility: Re-evaluate your loved one’s current income, assets, and medical needs against potential new eligibility criteria. Consult with an elder law attorney if you have complex financial situations or questions about asset protection.
- Understand HCBS Options: Research your state’s Home and Community-Based Services (HCBS) waivers and programs. Understand the application process, eligibility for specific services, and any waiting lists.
- Assess Technology Readiness: Evaluate your and your loved one’s access to and comfort with technology for telehealth and digital health tools. Identify any potential barriers and seek resources for digital literacy if needed.
- Maintain Meticulous Records: Keep organized, detailed records of all medical appointments, treatments, financial statements, and communications related to Medicaid. This is crucial for eligibility reviews and to demonstrate compliance.
- Connect with Support Networks: Join caregiver support groups, connect with local Area Agencies on Aging, or disability advocacy organizations. These networks can provide valuable peer support, information, and resources specific to your region.
- Advocate for Your Loved One: Be prepared to ask questions, challenge decisions, and advocate for your loved one’s needs within the evolving Medicaid system. Your voice is powerful.
- Financial Planning: If possible, consult with a financial advisor who understands Medicaid planning to ensure your loved one’s financial resources are managed effectively in light of potential rule changes.
- Understand Managed Care: If your state uses Medicaid Managed Care Organizations (MCOs), familiarize yourself with how they operate, the services they cover, and their complaint resolution processes.
- Be Patient and Persistent: Navigating government programs can be challenging. Patience, persistence, and a willingness to seek assistance when needed will be invaluable.
Conclusion: Empowering Caregivers in the Face of Change
The 2026 Medicaid Updates will undoubtedly bring a period of adjustment for family caregivers across the United States. While the specifics of these changes will continue to unfold, the overarching themes point towards a system that is striving for greater efficiency, improved outcomes, and expanded home-based care. For caregivers, this means a continued need for vigilance, adaptability, and proactive engagement with the healthcare system.
By understanding the potential shifts in eligibility, the growing emphasis on Home and Community-Based Services, the move towards value-based care, the integration of digital health, and strengthened anti-fraud measures, you can better prepare yourself and your loved one. These changes, while complex, also present opportunities for enhanced support and more person-centered care. Your role as a family caregiver is indispensable, and being well-informed is your most powerful tool in navigating the evolving landscape of Medicaid.
Remember, you are not alone in this journey. Utilize the resources available, connect with support networks, and advocate tirelessly for the well-being of those you care for. The future of Medicaid is being shaped, and your active participation in understanding and adapting to these changes will ensure that your loved one continues to receive the care and support they deserve.






